Managing and treating joint pain: Adding to the essentials
The treatments described in this chapter will probably sound more like ‘medical treatments’ than those described in chapter 4. They are not, however, meant to replace those essential ways of managing joint pain for which there is evidence of effectiveness – physical activity, suitable footwear, losing weight if overweight, heat and cold, and distraction and relaxation. If despite doing the essential basics you are still finding it difficult to manage, then you and your GP might want to talk about some of the following treatments.
-
Physiotherapy
A key message of this guidebook is that regular physical activity is an effective way of managing the symptoms of OA.
If, though, your symptoms get worse after doing appropriate physical activity, this does not mean that you should stop exercising but you may need to seek further advice. If you want an exercise programme tailored to your particular problem or simply want further advice and reassurance about taking exercise, then a physiotherapist can help.
Physiotherapists can devise suitable exercise programmes – land and water based – as well as advising more generally on aerobic exercise, such as walking and swimming. Physiotherapists also use manual therapy (manipulation and stretching) to help improve the working of joints affected by OA and to alleviate pain. This is especially effective for hip pain. Manual therapy is not usually offered on its own but as part of a package of care with exercise.
-
Electrotherapy
TENS (Transcutaneous Electrical Nerve Stimulation) is a machine that sends electrical pulses through the skin, which some people find helps relieve pain and stiffness. There are different makes and models of TENS with a range of prices. Physiotherapists can advise about the different kinds of machine and how best to use them.
While some individuals may experience a worsening of symptoms the vast majority of people, including those severely affected, will not have any adverse reaction to controlled exercise. For example, patients with significant osteoarthritis can ride a bicycle, go swimming or exercise at a gym with often no or minimal discomfort.
They may also be able to lend one out for a trial period. If a TENS machine does not seem to be helping then try experimenting with different pulse strengths and length of time of application.
-
Aids and devices
Walking aids
Walking aids are useful for some people, providing a feel of security and stability. Whilst some people don’t like the idea of using a walking stick because it makes them feel old, other options are available. Others feel that even if a stick is seen as a symbol of old age, the benefit it brings, in giving them the confidence to walk, outweighs the disadvantages.
“I used to walk very briskly. Well, I’m not doing so now. Mind you, as I say, I’m using a stick – in fact I’ve got two sticks but it makes me feel old and doddering if I have two. But I do find that it makes me a bit more sprightly if I’ve got a stick.”
A walking stick needs to be adjusted to the appropriate length for the user. The retailer supplying the stick should do this. Sticks come with different types of handles, so that people who have painful hands can select one that is most comfortable for them. The tip has a rubber grip to prevent the stick from slipping, which will need to be replaced from time to time.
Often, people are advised to use a walking stick on the side opposite to the affected leg, and that the stick and the affected leg should move forward together. Using a walking stick in this way reduces the pressure on the painful leg joint. However, some people use their stick as a ‘third leg’ in case their leg gives way, and to do this they use the stick on the same side as the leg with the problem. So, if the purpose of the walking stick is to help you reduce pressure on the hip or knee then use it on the side opposite to the affected leg. However, if the purpose is to improve your balance and to feel safer when walking then use the stick on the same side as the problem leg.
Recently there has been interest in the use of Nordic walking poles for people with OA of the hip or knee. A Nordic walking pole is longer than a walking stick and has a loop or grip for holding. They are used in a style of walking that is described as cross-country skiing without skis (or snow!). There are claims that posture and walking is improved, the pressure on knee joints is reduced, and more energy is burned during Nordic than ordinary walking. (So in theory Nordic walking could help with weight loss.)
Assistive devices and joint protection
There are lots of gadgets on the market to help with everyday tasks and hobbies. Some may prove to be useful and some may not. Joint protection approaches can be beneficial for hand pain and OA. Occupational therapists have particular expertise in this area. It is best to get advice before buying specialist equipment. Some local authorities, hospital trusts and voluntary organisations have set up independent living centres, (See Assist UK page 51), which do not sell equipment, but where there are people who can advise on the suitability of different products, and where equipment can be tried out.
Insoles, supports, splints and braces
In OA the joint may be out of line. Shoe insoles, braces for hip and knee, and thumb splints may help correct a misalignment and provide support. It is thought this can help decrease the pain and improve physical function. Physiotherapists, podiatrists (chiropodists) or occupational therapists can assess whether or not such products are suitable.
-
Medicines for managing pain
From a patient’s point of view, medicines are often the least preferred way to manage pain.
“I think you’re frightened of getting used to drugs and you rely on them. I’d rather take them when I really need them. At the moment I think I can cope all right.”
However, even when patients would ideally like to be able to manage without medicines, some find they need to take them.
“I used to stride out and I can’t do that anymore. I seem as though my joints are stiff. But if I take the tablets I get an easing…I get a loosening in my joints. Whether it’s because I don’t feel the pain, I don’t know but when I take them I’m a lot better.”
In the SMootH trial carried out by researchers at Keele University, people with hand OA who had joint protection education from occupational therapists were more likely to have improved than people who did not have joint protection. They also felt more confident in managing their hand pain.
Published by Dziedzic and colleagues in Annals of the Rheumatic Diseases 2015;74(1):108-18.

There are different types of medicine that can help manage pain from OA.
A group of medicines called non-steroidal anti-inflammatory drugs (NSAIDs) have both an analgesic and an inflammation-reducing effect. OA does not often involve inflammation, so it is mainly the analgesic effect of an NSAID that is beneficial to someone who has joint pain. NSAIDs come in a cream form that is applied to the skin over the affected joint – these are called topical NSAIDs. They also come in a tablet form to be taken by mouth.
Topical creams

NSAIDs in a cream form (topical NSAIDs)
While a few topical NSAIDs are available only on prescription, there are a number, most of them containing an NSAID called ibuprofen, which are on sale to the public. There is evidence that they may help relieve pain in knee and hand OA. They should be applied with a gentle massage, using only the amount specified on the information leaflet. (The massage alone can help ease pain.)
Pain relief is most effective during the first two weeks of using the cream. They can be used in conjunction with paracetamol. Topical NSAIDs are not associated with the side effects of NSAIDs taken by mouth, which are described below. For this reason health professionals think that topical NSAIDs are the preferable treatment for hand and knee OA.
Creams containing Capsaicin
An age-old remedy for painful joints is to rub in lotions which have a stinging effect. There is evidence that capsaicin cream, whose active ingredient is an extract of chillies, can help relieve pain. It may burn at first, but after several days use can give a useful numbing effect. It does not work for everyone, and for some the initial burning puts them off using it. However, it can be particularly effective for the small joints of the hand, such as the base of the thumb, as well as for knee OA.
Capsaicin is available in the UK on prescription only. It should be applied with gentle massage onto skin that is not inflamed or broken. Hot baths or showers should be avoided just before and just after applying it.
The use of topical NSAIDs or capsaicin, and along with regular exercising of affected joints, can help people to cope with flare ups of joint pain.
NSAIDs tablets
 Most NSAIDs that are taken by mouth are available only on prescription. Ibuprofen is an exception, for it is an NSAID that can be bought in shops and pharmacies. The pain-relieving effects of an NSAID should start to work quite quickly. If an NSAID is not having an effect on pain after a week or two, then it is probably not going to be effective.
Most NSAIDs that are taken by mouth are available only on prescription. Ibuprofen is an exception, for it is an NSAID that can be bought in shops and pharmacies. The pain-relieving effects of an NSAID should start to work quite quickly. If an NSAID is not having an effect on pain after a week or two, then it is probably not going to be effective.
NSAIDs have been in use for many years and have been associated with serious side effects. Diclofenac (brand names include Diclomax and Voltarol), and naproxen (brand names include Synflex) are examples of these older NSAIDs.
More recently a different type of NSAID, called a COX-2, has been developed which it was thought would have fewer side effects. Celecoxib (Celebrex) is an example of a COX-2. As more has been learned about the action of NSAIDs and COX-2 on the body, it has been realised that they are not as distinctly different as was first thought. (From now on the word ‘NSAID’ will refer to COX-2 as well as the older NSAIDs.)
NSAIDs can cause side effects, the most common of which is stomach problems. With long term use and high doses, NSAIDs, particularly the older type, can cause stomach ulcers or inflammation, which can cause bleeding. A medicine to lessen stomach problems is usually prescribed with an NSAID. NSAIDs can worsen kidney function and blood pressure control. Older people are more at risk than are younger people. They are also associated with a very small increased risk of heart attacks and strokes.
Ibuprofen taken in the dose and way recommended on the package is less likely to cause problems.
If any new symptoms develop while taking an NSAID, no more doses should be taken and advice should be sought from a doctor or pharmacist as soon as possible.
The advice that is given to doctors about NSAIDs is to prescribe the lowest effective dose for the shortest possible time to control symptoms.
They should be taken with or after food, as that reduces the likelihood of stomach side effects. Only one brand of NSAID should be taken at a time, and taking an NSAID along with a low dose of aspirin may increase the risk of stomach problems and reduce the benefit from the aspirin. For some people who have asthma, NSAIDs can bring on symptoms of asthma.
Paracetamol
Paracetamol is sometimes offered by doctors. For most adults, two 500mg tablets can be taken up to four times in 24 hours (do not take more than this because an overdose may cause irreversible damage to the liver). If paracetamol is not effective for you there are other medicines that your doctor may prescribe.
Opioids
Opioids are a type of painkiller that were first made from the juice of the opium poppy. Nowadays many are synthetic – they are manufactured in a laboratory. They are used for moderate to severe pain.
Some types of opioid are stronger than others. Morphine is an example of a strong opioid and codeine of a weak one. Some types of weak opioid can be bought over the counter at shops and pharmacies.
Long term use of opioid analgesics may cause people to become dependent on them. Some people have said they make them feel
‘woozy’. Constipation is also a common side effect with opioids taken by mouth. People should not drink alcohol when taking opioids.
Cortisone injections
An injection into a joint may give temporary benefit to those with moderate to severe pain.
Complementary and alternative medicine
Complementary and alternative medicine includes a wide range of therapies. Amongst the best known are acupuncture, osteopathy, chiropractic, homeopathy, herbal medicine, aromatherapy and massage. Surveys have found that complementary therapies are popular with people who have osteoarthritis-type joint problems.
Most people use this kind of treatment not to find a cure but to help ease the symptoms, particularly the pain, and so lead as normal a life as possible. Often they seek help from a complementary therapist after they have seen their doctor and have tried out any treatments offered there. Many people continue to see their GP alongside a complementary therapist.
Your GP should offer you an annual review if:
- your joint pain is troublesome
- you take tablets regularly for pain relief
- you have co-existing health problems
- your joint pain is at more than one site
Complementary medicine is seen by many who try it to have several advantages over conventional medicine:
- Complementary medicine often looks at a medical problem in the context of the whole person and does not focus solely on treating symptoms
- Concern that conventional medicine often involves taking drugs whose side effects may be as problematical as the symptoms they are treating
- Complementary therapists may have more time and take account of personal issues that might also be affecting a health condition
- Acupuncture is not recommended by NICE for the treatment of osteoarthritis. Osteopathy and homeopathy may be available on the NHS.
Two drawbacks to getting care from a complementary therapist are:
- Getting assurance that the therapist is reputable
- The cost
For all of the therapies listed below there is an official body which registers those that have undertaken a recognised course of training in their field. It is quite in order to phone a therapist before starting treatment to ask about the cost, the likely number of treatment sessions and details of what the treatment will involve.
Whether people continue to seek care from a complementary therapist or not depends on whether the therapy is felt to be effective. Most people adopt a try and see it approach; if the therapy does not seem to make any difference to their problem after four or five sessions they stop it, and perhaps try something else. (A therapy such as the Alexander Technique will require more than five sessions to teach the method.)
A list of common complementary therapies used by people with OA
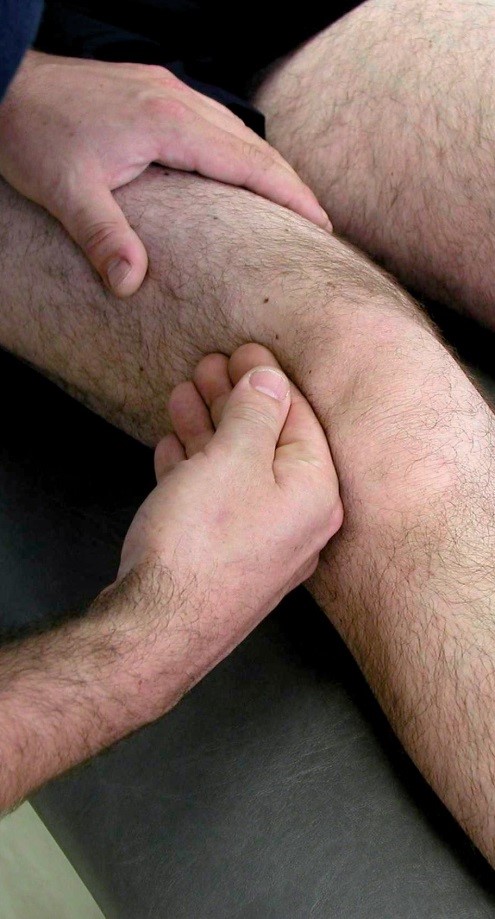
1. Chiropractic
Treatment consists of a wide range of manipulative techniques designed to improve the function of the joints, and so relieve pain and muscle spasm. Ice, heat or massage treatment may be recommended. Chiropractors also offer individual advice about lifestyle, work and exercise that help to manage the condition and prevent a reoccurrence.
2. Homeopathy
Based on the idea that the body is thought to naturally heal itself. Homeopathic medicines contain substances in very dilute form that cause the same symptoms as the problem being treated and which, it is claimed, stimulate the body’s healing process. Choice of remedy depends not only on the symptoms but also on the nature of the person who has the condition.
3. Osteopathy
Based on the notion that problems or pain associated with the structure of the body can also affect the working of the body. Osteopaths use their hands to stretch, massage and touch the body in a variety of ways using a mixture of gentle and forceful techniques. The aim for those who have OA is to increase the circulation and drainage from the affected joints, to reduce any inflammation present and to enable the joints to move as well as they are able to. This, it is thought, helps reduce the stress that is placed on the affected joints.
4. Alexander Technique
This is a movement therapy designed to identify posture problems in the body and to teach appropriate ways of standing, sitting and moving that reduce strain and muscular tension. Movements (to be practised at home) are taught, that aim to increase body awareness, correct posture and to help movement. Particular attention is paid to the way that the head is held and to freeing the spine and enabling muscles to lengthen.
Surgery
Most people who have OA will not need surgery. Usually joint replacement surgery is only considered when symptoms are having a substantial effect on an individual’s ability to do everyday activities, and after a patient has tried at least the basic forms of treatment described in chapter 4. If your doctor does not mention surgery, you should not assume that it has been ruled out. If you want to know whether joint replacement is something that might be appropriate in your case, you should ask directly. Surgeons recommend that patients be referred to them before developing prolonged disability and severe pain.
Sometimes people who are offered surgery do not take up the offer straightaway. This can be for a variety of reasons, including concerns about how they will carry out caring responsibilities during rehabilitation, and how long the artificial joint will last.
“And like I say because my sister was poorly I decided that I would put the operation off. –They tell you these knees only last ten to twelve years. Well I am sixty four this year, so if they last twelve years I am going to have to have it done again when I am seventy six.”
Do raise concerns such as these with a GP, so that they can form part of the discussion about whether or not it is appropriate and timely to be referred for surgery.
Things to remember
- Physiotherapists can devise tailor made exercise programmes and help support patients to continue with their exercises. They can also advise on the use of insoles, supports and braces, and TENS machines.
- Creams for hand and knee OA containing NSAID are the preferred medicine to manage pain. If these are not effective then doctors can prescribe other medicines, though there are concerns about the long-term use of some of these.
- There are many special gadgets to help with everyday tasks. Before buying take independent advice, and try out the equipment to make sure it is suitable.
- Many people try complementary therapies.
- Only a small number of people with OA will require surgery.